
A few days before I left for my short holiday to Fiji, I tripped on uneven paving where I grazed my elbow, and twisted my knee. These slight injuries were annoying but not enough to alter my plans – or should they have been? I could never have guessed that a small ‘graze’ might lead to atrial fibrillation!
I went to a Pharmacy the next day to buy some larger ‘band-aids’ to cover my elbow but otherwise prepared for my trip as usual. My flight was a few days later and I travelled to the airport by public transport. My knee bothered me a little but not enough to need any help with my luggage – I used a walking pole for some extra support.
My arrival in Fiji was uneventful and I caught a boat to the ‘island’, which was to be my ‘paradise home’ for seven days. Unfortunately, I soon discovered that the warm tropical water inflamed the graze on my elbow so for most of the time I avoided exposing it to sea water. I could still paddle with my arm held above the water and I was rigorous about cleaning and re-dressing the graze. For this I had the advice of a (holidaying) medical practitioner and the first aid officer. There was little change in seven days – the graze became neither any worse nor any better.

Sunset from the verandah of my Bure at Barefoot Manta Island
The day after I left the island for home, I spent one day at Denarau. I went to the Pharmacy to get more ‘band aids’ but the pharmacist suggested that I should apply a cream to the graze. This seemed to be absorbed extremely rapidly and I later found out that this same cream has been previously associated with Atrial Fibrillation. But did the cream somehow cause my later problems or was it just the heat?
Within about 30 minutes of applying the cream, my arm was noticeably swollen and within a couple of hours I had obvious cellulitis, which became very severe (see Photo below). I went to the Fijian Emergency Medical Service where I was given antibiotics but possibly too low a dose?
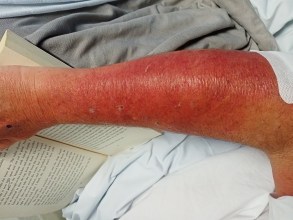
In hospital with my arm, swollen and red with Cellulitis
The following morning, I had an early flight back to Sydney. I made it home and rested till the next day, when I had an appointment with my General Practitioner. My GP immediately referred me to the Emergency Department at the local hospital for intravenous antibiotics but when I arrived, they admitted me straight away because my pulse was extremely high, and my heart was in Atrial Fibrillation (AFib). So, I came home from hospital four days later, having become a ‘Cardiac Patient’. I had a Cardioversion operation but unfortunately, the normal rhythms didn’t remain, and I am now on heart medications for (probably) the long-term.
Incidentally, the IV antibiotics cleared the Cellulitis quite quickly and no one seemed the least bit interested in that!
As I knew nothing about AFib before my recent ‘adventure’, I thought I’d write a little about it. Apparently AFib is extremely common as we age and is a major cause of stroke.
Atrial Fibrillation in an apparently healthy person
Diagnosing atrial fibrillation (AFib) in a healthy person can be challenging since AFib is typically associated with certain risk factors and medical conditions. Atrial fibrillation is an irregular and often rapid heart rate that can increase the risk of stroke, heart failure, and other heart-related complications. It is more commonly observed in older individuals and those with underlying heart conditions or other risk factors. Infection can cause atrial fibrillation (AFib) through several mechanisms, though the exact reasons may vary depending on the type and severity of the infection. AFib triggered by infection is often referred to as “secondary” or (sometimes) “postoperative” AFib, as it may occur as a complication of an underlying infection or a surgical procedure. Some of the common ways infections can lead to AFib include:
- Inflammation and Electrical Disturbances: Infections can cause a significant inflammatory response in the body. The release of inflammatory substances can disrupt the normal electrical signals in the heart, leading to abnormal heart rhythms, including AFib.
- Autonomic Nervous System Imbalance: Infections can affect the autonomic nervous system, which controls the heart’s rate and rhythm. Imbalances in the autonomic nervous system due to infection may promote the development of AFib.
- Fluid and Electrolyte Imbalance: Severe infections, especially those affecting the respiratory system, can lead to dehydration and imbalances in electrolytes (e.g., potassium, magnesium). These imbalances can directly influence the heart’s electrical activity and contribute to AFib.
- Increased Sympathetic Nervous System Activity: Some infections can increase sympathetic nervous system activity, leading to an increased heart rate and potential arrhythmias, including AFib.
- Ischemia and Myocarditis: Certain infections can cause inflammation of the heart muscle (myocarditis) or lead to reduced blood flow to the heart (ischemia). These conditions can disrupt the heart’s electrical conduction system, potentially leading to AFib.
- Medications and Treatment: Some medications used to treat infections, such as antibiotics and antivirals, can have side effects that affect the heart’s rhythm and increase the risk of AFib.
It’s essential to recognize that not all infections will cause AFib, and the risk of developing AFib due to an infection can vary among individuals based on their overall health, existing heart conditions, and other risk factors. Infections that are severe, widespread, or affect vital organs are more likely to increase the risk of AFib and unfortunately the AFib is likely to remain. In a healthy person without any known heart conditions or risk factors, diagnosing AFib may require detecting its presence during routine health checkups or through an incidental finding during an electrocardiogram (ECG or EKG) for another unrelated issue.
In my case, I am fairly sure I didn’t have AFib before this apparent infection. I say ‘apparent’ because I did not have a fever and the laboratory did not identify any infectious ‘agent’. Unfortunately there are no lifestyle modifications I can make other than giving up my glass of wine at night – and I’m not sure that I need to do that! As you probably know, I have written books about healthy ageing and cancer prevention, I don’t smoke, I have an excellent diet, I’m fairly relaxed, and I exercise regularly – so I guess I have to live with it (and the medicines) – although I would appreciate any realistic suggestions.